The Postpartum Sleep Paradox: Why New Mums Are Built to Sleep Less
Why Nature Thinks Sleep-Deprived Mothers Are not Such a Bad Idea
A few months ago, I published the sleep blueprint. I told you the truth: sleep is the non-negotiable foundation. The glymphatic system clears waste from your brain overnight. REM sleep processes your emotions. Miss enough of it and your biology ages faster than your calendar.
And then I added a footnote, almost as an aside.
If you’re in the thick of early motherhood, that information might feel like an accusation. Here’s what I want you to know: we are biologically designed to rear children.
That means not sleeping well for a period of your life. It’s temporary.
Several of you wrote in asking a version of the same question: if sleep is so critical, why does nature build new mothers to be chronically deprived of it? Was evolution asleep on the job?
This post is the answer to that question.
It’s a Zoom post. No protocols. No hacks. Just the mechanism behind why this happens, what your biology is actually doing in those exhausted first months, and why the science is more reassuring than the headlines suggest.
New here? Start here:
Swiss Army Mum is a practical guide to long-term health for busy women, built on four pillars: Body, Mind, Glow, and Flow.
Not every tool. Just the right ones.
The Paradox
Start with the stakes.
Mothers sleeping fewer than seven hours a night at six months postpartum show epigenetic markers that suggest their cells are between three and seven biological years older than those of better-rested peers1. That’s not a typo. Six months of poor sleep can age you, at the cellular level, by up to seven years.
And yet: every mammal on earth does this. Every new mother wakes through the night. Every marmoset, every rat, every wolf mother rearranges her sleep for her offspring. This has been happening for tens of millions of years, across wildly different species and environments.
If postpartum sleep disruption were simply a mistake, selection pressure would have fixed it by now. It hasn’t. Which means either nature is extraordinarily indifferent to maternal health, or something more interesting is going on.
The evidence points to something more interesting.
This Is Not a Bug
Sleep fragmentation in new mothers is not a failure of the system. It’s a feature of a different system, one built around infant survival rather than maternal optimization.
Think of it like a factory that temporarily redirects its energy grid. Under normal conditions, the factory runs full production for itself: building, repairing, maintaining. When a critical external demand arrives, power gets redirected. Output elsewhere drops. Efficiency suffers in some departments. But the priority gets met.
Your biology, in early motherhood, is running a version of that redirect.
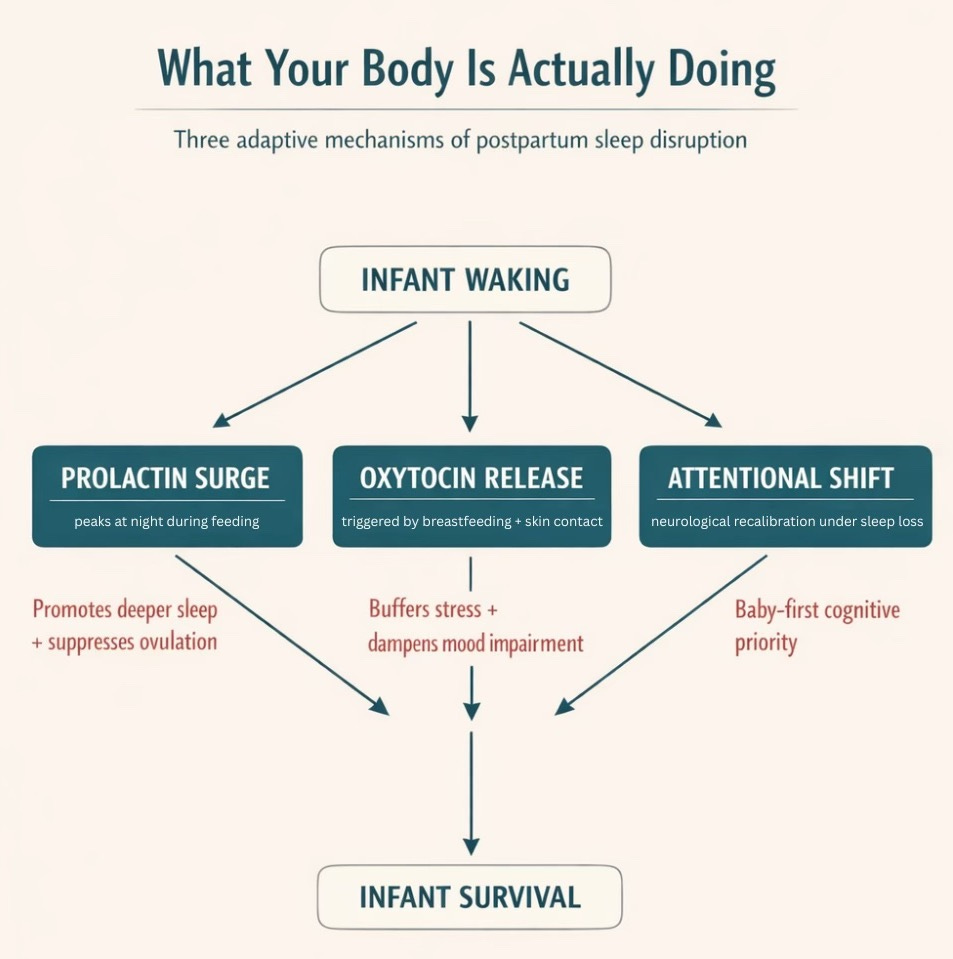
The Attentional Shift
The first thing sleep deprivation does to new mothers is not what it does to everyone else.
In most people, sleep loss blunts attention, slows reaction time, and creates a general fog. In new mothers, something more specific happens. A study of first-time mothers found that those sleeping fewer than seven hours a night were significantly faster and more accurate when responding to infant-related cues compared to self-related ones2. Well-rested mothers showed no such bias. Their attention was distributed more evenly.
The sleep-deprived mothers, in other words, had been recalibrated. Cognitive resources were scarce, so the system redistributed them. Baby first. Everything else later.
This is not a metaphor for maternal love. It’s a measurable neurological shift. When you’re running on four hours of fragmented sleep and your infant makes a sound, your brain is primed to respond before you’re consciously aware of it. That’s the system doing exactly what it was built to do.
It’s worth noting the flip side: untreated insomnia in parents, the kind that persists beyond early infancy without that protective biological context, is linked to less sensitive caregiving3. The adaptive vigilance of early postpartum sleep loss is not the same thing as general sleep deprivation. The biology has a context.
Oxytocin: The Stress Buffer
New mothers also have a hormonal advantage that non-mothers don’t.
Oxytocin, released during breastfeeding and skin-to-skin contact, is best known as a bonding hormone. But it’s also anxiolytic: it actively dampens the stress response. Women with higher oxytocin levels before a sleep disruption event showed measurably less mood impairment the following day compared to women with lower levels4.
This is not a small effect. It suggests that the same physiological process that feeds your baby is also quietly buffering you against the emotional consequences of the broken night that feeding caused.
Prolactin works alongside it. The hormone that drives milk production peaks at night and appears to promote deeper sleep during the windows when sleep does happen5. Your body seems to be building in a mechanism: wake up to feed, but when you do sleep, make it count.
The result is a sleep architecture that looks terrible on paper but is more functional than the raw numbers suggest. You’re getting less sleep. You’re also getting a hormonal environment that is, to some degree, purpose-built to help you cope with getting less sleep.
The Evolutionary Logic
Zoom out further and the picture gets more interesting.
Infant sleep disruption is almost certainly adaptive for the infant as well as for the mother. Frequent night waking suppresses ovulation through elevated prolactin, extending the inter-birth interval and concentrating parental investment on the current offspring6. One model proposes that postpartum depression, when it co-occurs with high infant night-waking, may function as a signal that triggers support-seeking from others in the social group, in effect broadcasting that the mother is overloaded and needs help7.
These are speculative frameworks. They’re evolutionary hypotheses, not established mechanisms. But they point toward the same conclusion: this system was not designed to be endured alone.
Marmoset mothers with newborns are awake more than three times as often at night as mothers without infants, and this elevated wakefulness persists for at least nine weeks8. That’s not a human quirk. It’s a mammalian pattern.
And in all mammalian species that have been studied, the solution to that pattern has never been individual maternal toughness. It has been social support.
The Modern Mismatch
Here’s where things get uncomfortable.
For most of human evolutionary history, new mothers were not doing this alone in a darkened room in a nuclear family household. They were embedded in multigenerational groups where night duties were shared, where other adults heard the infant, where sleep could be recovered in distributed fragments across a social network.
The anthropological evidence suggests that co-sleeping, alloparenting (care by non-parents), and communal overnight support were the norm rather than the exception in ancestral environments9. The biology adapted to a context where help was available.
Modern isolation is the mismatch. The physiological machinery is not designed to run indefinitely without external support. When researchers look at what actually reduces the health consequences of postpartum sleep loss, the most consistent finding is partner and family involvement in night care. Even occasional relief, a single long block of sleep, a shared feed, a nap while someone else is present, meaningfully reduces sleep debt and its downstream effects.
The answer to the postpartum sleep paradox is not that your body is broken.
It’s that your body was built for a village.
What This Means Practically
A few things follow from the biology.
The fragmentation itself may be less damaging than it looks. One controlled experiment found that a single night of simulated postpartum-like awakenings, three interruptions of roughly thirty minutes each, did not impair psychomotor performance the following day despite subjective reports of poor sleep10. Acute fragmentation, in a context where the rest architecture is otherwise intact, appears more tolerable than chronic total sleep restriction. This doesn’t mean sleep deprivation isn’t real. It means the body has some short-term buffering capacity that most of us don’t give it credit for.
Sleep timing matters more than most new parents realise. Going to bed earlier and keeping a consistent bedtime, even if wake times are unpredictable, is associated with measurably better daytime performance.
If you can do one thing, consistency is it.
Breastfeeding doesn’t shorten your sleep. A large longitudinal study found that breastfeeding itself was not independently associated with reduced maternal sleep duration. What correlated with shorter sleep was the number of feeds.The mechanism is the number of wakings, not the method of feeding. This matters because the oxytocin and prolactin benefits of nursing are real, and the decision to breastfeed should not be driven by fear that it’s making the sleep worse.
The biology is temporary. The cellular aging data is real, but it reflects a specific window. As infant sleep consolidates, the maternal system recovers. The redirect ends, the factory returns to full production, and the biological clock can be wound back. Early postpartum sleep loss does not permanently compromise your health if it is followed by recovery.
And if the postpartum months were brutal for you, physiologically brutal, not just hard in the way people warn you it will be hard: that is data. It means you were running the system without sufficient support, in a context it was not designed for. That’s not weakness.
It’s a modern structural problem wearing the costume of a personal one.
A Note to Non-Mothers
This post is about postpartum biology, but the mechanisms are relevant more broadly.
Oxytocin as a stress buffer during sleep disruption. Circadian consistency as a lever for function under fragmentation. The role of social support in recovery. These are not exclusive to new parents. They are general principles about how sleep interacts with stress, hormones, and social context.
If you’re in a period of disrupted sleep for any reason, the lesson from postpartum biology is not that you should just push through. It’s that your body has more adaptive capacity than you think, that consistency matters more than total hours in the short term, and that trying to do it alone makes everything harder than it needs to be.
Your Turn
Were you a new parent who felt the weight of sleep research as guilt rather than guidance? Or did you come through it and want to share what actually helped?
Drop a comment. I read every one.
Thank You
Thank you for reading, sharing, and supporting this work. Whether you’ve been here since the beginning or just found Swiss Army Mum, I’m glad you’re here.
Building sustainable health without overwhelm takes a village. If something resonated with you, I’d be grateful if you forwarded this to someone who might benefit or hit the ♥️ or ↻ Restack button. It helps more people discover this space and build sustainable health without the overwhelm.
Medical note: This is educational, not personal medical advice. Your biology, history, and context matter. Work with a qualified healthcare professional.
References
Carroll, Judith E et al. “Postpartum sleep loss and accelerated epigenetic aging.” Sleep health vol. 7,3 (2021): 362-367. https://doi.org/10.1016/j.sleh.2021.02.002
Hoegholt NF, Buus S, Stevner ABA, Sui J, Vuust P, Kringelbach ML. Sleep-deprived new mothers gave their infants a higher priority than themselves. Acta Paediatr. 2023 Jan;112(1):93-99. https://doi.org/10.1111/apa.16560
King LS, Rangel E, Simpson N, Tikotzky L, Manber R. Mothers' postpartum sleep disturbance is associated with the ability to sustain sensitivity toward infants. Sleep Med. 2020 Jan;65:74-83. https://doi.org/10.1016/j.sleep.2019.07.017
Astbury L, Bennett C, Pinnington DM, Bei B. Does breastfeeding influence sleep? A longitudinal study across the first two postpartum years. Birth. 2022 Sep;49(3):540-548. https://doi.org/10.1111/birt.12625
Haig D. Troubled sleep: Night waking, breastfeeding and parent-offspring conflict. Evol Med Public Health. 2014 Jan;2014(1):32-9. https://doi.org/10.1093/emph/eou005
Gunst, Annika et al. “Postpartum depression and mother-offspring conflict over maternal investment.” Evolution, medicine, and public health vol. 9,1 11-23. 2 Jan. 2021, https://doi.org/10.1093/emph/eoaa049
Fite, J.E., French, J.A., Patera, K.J. et al. Nighttime Wakefulness Associated with Infant Rearing in Callithrix kuhlii . International Journal of Primatology 24, 1267–1280 (2003). https://doi.org/10.1023/B:IJOP.0000005992.72026.e6
Hrdy, Sarah Blaffer. Mothers and Others: The Evolutionary Origins of Mutual Understanding. Harvard University Press, 2009. https://doi.org/10.2307/j.ctt1c84czb
McBean AL, Kinsey SG, Montgomery-Downs HE. Effects of a single night of postpartum sleep on childless women’s daytime functioning. Physiol Behav. 2016 Mar 15;156:137-47. https://doi.org/10.1016/j.physbeh.2016.01.014




