Much Ado About Peakspan: Staying Close to your Peak for Longer
A 2026 longevity paper introduces a concept worth knowing. Not because it's proven. Because the data behind it backs the whole point of the SAM system.
If you’re new here, hi!
Swiss Army Mum is a simple, science-based wellness system for busy women. Four pillars. No overwhelm.
Not every tool. Just the right ones.
A few years ago, I had a routine physical. Everything came back normal. My doctor was pleased. Fasting glucose, fine. Cholesterol, fine. Blood pressure, fine. “You’re in good health.”
I walked out feeling like I should be relieved. But something was nagging at me.
My recovery from hard workouts was slower than it used to be. I needed more sleep to feel the same level of alert. My body composition had shifted even though my diet hadn’t. I was slower to learn new physical skills than I had been at 30. Nothing was wrong. But something had clearly changed.
Here’s what my doctor didn’t say, because it is not what annual physicals are designed to tell you: I was already years into physiological decline across multiple systems. Not diseased. Not even close. But measurably below where I had been at my biological best.
A perspective paper published in Aging and Disease in early 2026 puts a name to this state. It’s called Peakspan1.
I want to be clear about what this paper is, and what it isn’t. And then I want to show you why the data behind the concept fits with everything in this system.
The Paper and Its Limits
Zhavoronkov, Ying, and Wilczok introduce Peakspan as a framework: the age interval during which a person maintains at least 90% of their peak functional performance in a specific domain. It is a perspective piece, not a clinical trial. No new data. No methods section. The bar for peer review is lower than for original research.
The lead author, Alex Zhavoronkov, runs Insilico Medicine, an AI drug discovery company whose business model rests on biological aging tools. The paper’s proposed solutions reference his company’s products by name. He discloses this. It does not invalidate the framework, but it means you should read it as a commercially-adjacent proposal, not a neutral scientific report.
The 90% threshold is also, by the authors’ own admission, arbitrary. “Provisional,” they write. The headline table of Peakspans across organ systems, which has been widely shared, is explicitly labeled “for illustrative purposes rather than as precise quantitative estimates.”
So: not a breakthrough discovery. Not a validated clinical tool. The hype is ahead of the evidence.
What it is: a useful synthesis of well-established data, assembled into a frame that sharpens the question. And the underlying science it draws on is solid. I cross-referenced the key claims against primary literature before including them here.
The Gap Nobody Measures
Here is the core observation, stripped of jargon.
Most biological systems peak in early adulthood. Cardiovascular fitness, raw cognitive processing speed, muscle strength, hormone output, the immune system’s fresh-cell reserves: all of them reach their apex somewhere in the 20s to mid-30s. Then they begin a slow, largely silent decline.
By the time chronic disease appears, the typical woman in her 60s or 70s has often been declining for 30 to 40 years. The disease is the endpoint of a very long trajectory.
But here is the point I want to make, because it is different from how wellness is usually framed.
The goal was never just avoiding disease. Everybody wants to avoid disease. That is not a particularly interesting goal to organise your health decisions around. The more interesting question is: what is the slope doing?
Between peak function and the first clinical diagnosis sits most of your adult life. That stretch is not neutral ground. It is a continuous drift downward through what the Peakspan authors call a “healthy but declined” state. Labs normal. Doctor unconcerned. Functioning, just not as well as you once did.
Think of it like this. You start your adult life with a full battery. Disease is when the device stops working. But there is a very long middle stretch where the battery reads 70%, 60%, 50%, and you are still getting through the day, still told by every test that you are fine. The device works. It just works less well than it used to.
The question worth asking is not “how do I avoid the battery dying?” The question is: how do I keep the battery close to full for as long as possible, so that the final drop is short, late, and fast rather than long, early, and slow?
That is what changing the slope means. And that is what the SAM system is actually designed to do.
What the Data Actually Shows
Here is what the published literature says, system by system. The Peakspan paper synthesises these trajectories; the individual studies are well-established.
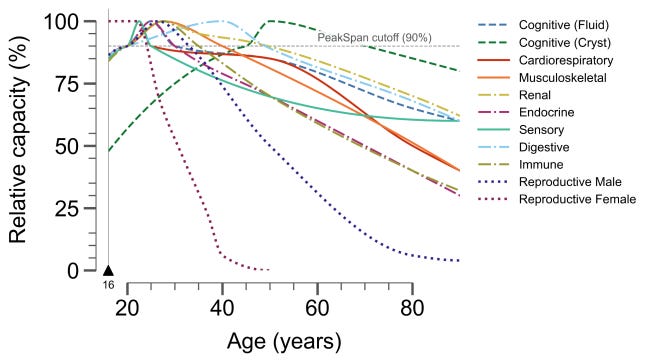
Cardiovascular fitness. VO2max, your maximal aerobic capacity and one of the strongest predictors of lifespan, peaks in the mid-20s and declines with age2. It does not plateau. It falls continuously, faster as you age.
Muscle strength. Peak knee extension torque is reached around age 20-28. For women, statistically significant decline begins at 40 to 50 and accelerates substantially between 60 and 70. Grip strength in women holds longer, plateauing until the mid-50s, but the underlying losses in muscle quality start earlier than the grip test reveals.
Fluid cognition. Processing speed, working memory, visual-spatial reasoning: these peak between age 20 and 243. After that, the decline is gradual but continuous. You are at your fastest and most computationally efficient at an age when most women have not yet figured out what they want to do with their lives.
Hormones. More on this in the next section, because female hormonal decline has a different shape from every other system on this list.
Kidney function. Glomerular filtration rate, the measure of how efficiently your kidneys filter your blood, starts declining in the early 30s and accelerates after 45. No symptoms. The decline is silent.
Immune function. Naive T-cells, the immune system’s fresh recruits that have never encountered a specific pathogen, peak before puberty and are already falling steeply by age 20. Thymic output falls to around 5% of its pre-puberty level by 55. This is part of why older adults respond less robustly to novel infections and new vaccines.
Plot all of this together and you see a cascade of systems beginning their descent in the 20s and 30s, while the clinical events medicine focuses on appear decades later. The gap between the two is most of your adult life.
Why Women Need a Different Map
The paper makes a point that Stacy Sims has been making for years: female physiology requires separate models, not adjusted versions of male ones.
For most systems, men and women follow qualitatively similar trajectories, with differences in timing and rate. But for the endocrine system, the shape of the curve is completely different.
Male testosterone declines gradually, roughly 1% per year, for decades. Female estradiol holds relatively stable through the peak reproductive years, then drops sharply and permanently at the menopausal transition4. The authors note this is a “qualitatively different trajectory,” not just a quantitative shift.
This matters because estrogen was not only a reproductive hormone. It was a systems manager, coordinating insulin sensitivity, muscle protein synthesis, bone turnover, inflammatory regulation, cardiovascular function, and aspects of cognitive processing. When it drops, those systems lose a coordinating signal that influenced a remarkable number of downstream processes.
The menopausal transition is therefore not just a hormone event. It is an inflection point across multiple Peakspan trajectories simultaneously.
What Actually Moves the Slope
Here is the honest version.
Some of these declines are not reversible. You are not going to restore the VO2max of a 25-year-old. Postmenopausal estradiol levels are what they are, and no lifestyle intervention restores them to premenopausal levels.
But the slope is modifiable. And the slope is what determines whether you are functional, strong, sharp, and independent at 75, or not.
A 10% per decade decline in VO2max in a sedentary woman produces a very different outcome at 70 than a 5% per decade decline in a woman who trains consistently. The line ends at the same wall, but it hits it later and from a higher starting point. That is the difference between independence and dependence in your final decade.
Cardiovascular fitness
Zone 2 cardio builds mitochondrial density and aerobic base. HIIT boosts VO2max directly. Two 10-minute sessions per week and 150 minutes of moderate cardio is 1.7% of your week.
Muscle strength and bone density
Progressive heavy resistance training is the most powerful tool for slowing musculoskeletal decline. The LIFTMOR trial5 showed that twice-weekly heavy lifting with impact loading improved bone mineral density in postmenopausal women with osteopenia. Not maintained it. Improved it.
Bone density via impact
Ten maximum vertical jumps, three times per week, significantly improved hip bone mineral density over six months6. Less than two minutes of actual jumping per week.
Fluid cognition
Aerobic exercise increases BDNF, the brain’s growth and repair signal. Sleep is when the glymphatic system flushes metabolic waste. Glucose stability reduces neuroinflammation. None of these reverse the underlying decline trajectory, but all of them slow it.
The endocrine system
This is where I want to be precise, because the answer is neither “nothing works” nor “exercise fixes everything.”
You cannot reverse the menopausal estrogen drop with lifestyle. That is true.
But Sims’ work in Next Level7 makes a specific, evidence-grounded argument: brief, intense exercise provides a metabolic and hormonal stimulus that partially substitutes for what declining hormones no longer deliver. HIIT increases human growth hormone and testosterone, decreases estrone (the less favourable form of estrogen produced by fat tissue), and counteracts cortisol when done at two sessions per week. Heavy strength training maintains the anabolic signalling that estradiol used to support.
The mechanism is not restoration. It is substitution. You are not replacing estrogen. You are finding other routes to some of the same downstream effects: muscle maintenance, metabolic function, bone protection. The routes are less efficient without the hormonal environment of your 30s. That is precisely why the dose matters more after 40, not less.
Think of it like this. Estrogen was the main power grid feeding those systems. It has gone offline. HIIT and heavy lifting are the backup generator you have plugged in. Not as seamless. Not as comprehensive. But the lights stay on.
The One Piece of Good News
Not every system follows the same downward slope.
Fluid cognition declines early. But crystallized intelligence, your accumulated knowledge, judgment, vocabulary, verbal reasoning, and pattern recognition built from decades of experience, peaks between ages 45 and 54. It remains relatively stable until around 80.
This is not a consolation prize. It is a distinct cognitive asset. The kind of thinking that requires experience rather than raw speed, that involves integrating complex information, navigating ambiguity, and knowing which questions to ask before rushing to an answer: that is where older expertise genuinely outperforms younger speed.
You are losing processing speed. You are gaining judgment. The goal is to protect both as long as possible.
The SAM Angle
Here is what Peakspan actually changes, if you let it.
Most healthcare advice is designed for the sick: manage your cholesterol, control your blood pressure, reduce disease risk. Most longevity content is designed for the worried-but-healthy: biohacking protocols, expensive tests, targeting the last 1% of variance.
SAM is designed for the gap. The 20 to 30 years between when biological decline begins and when clinical disease appears. That gap is not neutral ground. It is where the slope is set. It is where the trajectory becomes destiny.
The Peakspan framework does not change what SAM recommends. It sharpens why it matters, and what you are actually aiming for.
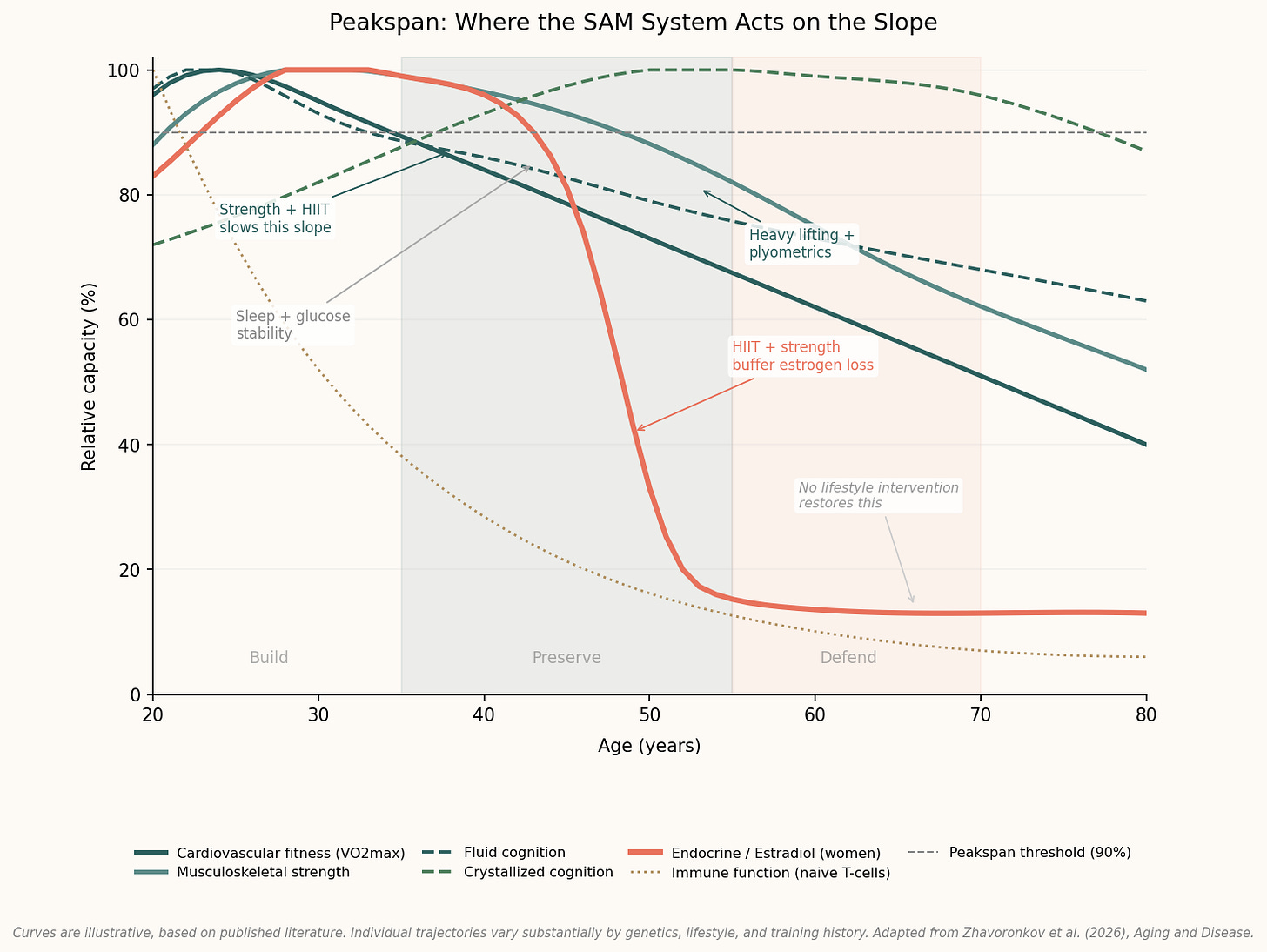
Sleep is not just about feeling rested. It is about slowing the cognitive and metabolic slope while you are still near the top of it. Heavy lifting is not about looking strong. It is about staying close to peak musculoskeletal function for as long as possible. Glucose stability is not just about avoiding diabetes eventually. It is about protecting systems that are already declining from the additional damage that chronic spikes layer on top.
The goal was never zero disease at age 90. The goal is a long plateau close to your best, followed by a short, late decline. Strong, sharp, and functional through most of your life, and a fast ending rather than a long one.
Changing the slope is how you get there.
A Note on the Research
The Peakspan concept comes from Zhavoronkov, Ying, and Wilczok (2026), published in Aging and Disease. As I flagged earlier, the lead author has commercial interests in the tools the paper proposes. The framework is speculative and the 90% threshold is provisional. What I have used from the paper is its synthesis of existing peer-reviewed data on functional decline trajectories, each cross-referenced independently. The individual references are solid. The unified frame is suggestive, not proven.
Your Turn
What function do you notice has shifted in the last five years, even though nothing is technically wrong?
Comment below. I read every one!
Thank you
Thank you for reading, sharing, and supporting this work. Whether you’ve been here since the beginning or just found Swiss Army Mum, I’m glad you’re here.
Building sustainable health without overwhelm takes a village. If something resonated with you, I’d be grateful if you forwarded this to someone who might benefit or hit the ♥️ or ↻ Restack button. It helps more people discover this space.
Medical note: This is educational, not personal medical advice. Your biology, history, and context matter. Work with a qualified healthcare professional.
Zhavoronkov A, Ying K, Wilczok D. Peakspan: Defining, Quantifying and Extending the Boundaries of Peak Productive Lifespan. Aging and Disease. 2026. https://doi.org/10.14336/AD.2026.0080
Letnes, Jon Magne et al. “Age-related decline in peak oxygen uptake: Cross-sectional vs. longitudinal findings. A review.” International journal of cardiology. Cardiovascular risk and prevention vol. 16 200171. 13 Jan. 2023, https://doi.org/10.1016/j.ijcrp.2023.200171
Hartshorne, Joshua K, and Laura T Germine. “When does cognitive functioning peak? The asynchronous rise and fall of different cognitive abilities across the life span.” Psychological science vol. 26,4 (2015): 433-43. https://doi.org/10.1177/0956797614567339
El Khoudary, Samar R et al. “The menopause transition and women’s health at midlife: a progress report from the Study of Women’s Health Across the Nation (SWAN).” Menopause (New York, N.Y.) vol. 26,10 (2019): 1213-1227. https://doi.org/10.1097/GME.0000000000001424
Watson, Steven L et al. “High-Intensity Resistance and Impact Training Improves Bone Mineral Density and Physical Function in Postmenopausal Women With Osteopenia and Osteoporosis: The LIFTMOR Randomized Controlled Trial.” Journal of bone and mineral research : the official journal of the American Society for Bone and Mineral Researchvol. 33,2 (2018): 211-220. https://doi.org/10.1002/jbmr.3284
Kato, Takeru et al. “Effect of low-repetition jump training on bone mineral density in young women.” Journal of applied physiology (Bethesda, Md. : 1985)vol. 100,3 (2006): 839-43. https://doi.org/10.1152/japplphysiol.00666.2005










This is such an important article. I know it. But I'm scared to read it right now, because I'm sure I'm there. Oy.